Pandemic Update, Hawaii and the World

Hawaii Covid 19 Update; cases continue to climb
The new variant has sent U.S. infections soaring, but a smaller share than with delta are resulting in hospitalization.
Healthy, boosted people unlikely to develop severe omicron infections, but with age there are greater health risks…
Healthy individuals who have been vaccinated, and especially those who have been boosted, appear unlikely to develop severe infections from the omicron variant that would land them in the hospital, say medical experts who have monitored the effects of the newest coronavirus variant since it was identified over four weeks ago.
While omicron has sent U.S. infections soaring to levels not seen since last winter’s wave, it appears to have less severe effects than the delta variant, according to a handful of international studies and early data from several U.S. hospitals.
Those infected by the omicron variant are 15 to 20 percent less likely to go to an emergency room, and 40 percent less likely to be hospitalized overnight, compared with those infected with delta, according to English data analyzed by scientists from Imperial College London. That aligns with early U.S. data from some hospitals.
At the Houston Methodist hospital system, about 15 percent of symptomatic individuals have ended up hospitalized — around a 70 percent reduction compared with those infected by the delta variant, said James Musser, chair of pathology and genomic medicine.
Other factors; age, preexisting conditions, vaccine type
Omicron poses a greater risk based on an individual’s age and the type of vaccine or booster they received, whether they have underlying health problems, such as heart disease or obesity, said Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota and a member of President Biden’s covid-19 transition task force.
“Have you previously had infection? Were you vaccinated? How many doses of vaccine, and was it more than six months ago? So in some ways this is almost like a calculus problem. It’s got a lot of moving parts to it and we’re trying to figure it out
Doctors also caution that far more people will become infected with Omicron simply because of its transmissibility.
If even a small fraction of those land in the hospital, they worry that health care systems that are already short-staffed because of delta infections could be overwhelmed — with potentially dire results for those needing critical care as a result of car accidents, heart attacks, strokes, or any number of things that bring people to emergency rooms.
“We need to be respectful of the fact that our hospital system has been under this kind of duress for such a long time,” said Larry Corey, a virologist at the Fred Hutchinson Cancer Research Center in Seattle. “We need to do everything we can to not allow the situation, where there’s such crowding and such intensity that we can’t optimally take care of the people who get severe disease.”
Pfizer pill becomes 1st US-authorized home COVID treatment
U.S. health regulators on Wednesday authorized the first pill against COVID-19, a Pfizer drug that Americans will be able to take at home to head off the worst effects of the virus.
The long-awaited milestone comes as U.S. cases, hospitalizations and deaths are all rising and health officials warn of a tsunami of new infections from the omicron variant that could overwhelm hospitals.
The drug, Paxlovid, is a faster way to treat early COVID-19 infections, though initial supplies will be extremely limited. All of the previously authorized drugs against the disease require an IV or an injection.
An antiviral pill from Merck also is expected to soon win authorization. But Pfizer’s drug is all but certain to be the preferred option because of its mild side effects and superior effectiveness, including a nearly 90% reduction in hospitalizations and deaths among patients most likely to get severe disease.
So far, according to a report issued ahead of peer review and updated on Monday, they see “no evidence of Omicron having lower severity than Delta, judged by either the proportion of people testing positive who report symptoms, or by the proportion of cases seeking hospital care after infection.”
Researchers at Imperial College London compared 11,329 people with confirmed or likely Omicron infections with nearly 200,000 people infected with other variants.
Hawaii Pandemic News
Hawaii reported three additional COVID-related fatalities on Saturday, Dec. 18th, pushing the death toll from the virus to 1,070.
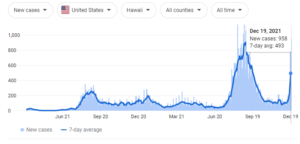 The state also reported 707 new cases. The latest infections bring the state’s total number of cases since the start of the pandemic to 91,744.
The state also reported 707 new cases. The latest infections bring the state’s total number of cases since the start of the pandemic to 91,744.
Over the last 14 days, the state says there have been 3,417 cases detected.
Amid an alarming increase of 797 new COVID infections, and DoH reported Omicron is among the case increases. Governor Ige and health leaders are urging the public to be vigilant and take additional precautions such as getting vaccinated or a booster shot.
Of the new infections reported Saturday:
- 622 were on Oahu
- 32 on Maui
- 22 on Hawaii Island
- 22 on Kauai
First Omicron Covid Variant Case Is Detected In Hawaii
The patient was not vaccinated and had no history of out-of-state travel, indicating it’s a case of community transmission. The Omicron variant confirmation comes as Hawaii has begun easing Covid-19 restrictions, the result of a statewide caseload which has largely leveled off after a surge sparked by the delta variant over the summer. Health officials reported 126 cases and one new death on Thursday, Dec. 2, 2021.
Currently, the state is averaging more than 350 cases a day. Some health officials believe cases will reach the thousands before 2021 is over and said more needs to be done before hospitals reach capacity.
The delta and omicron variants continue to spread across Hawaii, and Dr. Scott Miscovich, Premier Medical Group founder, said Saturday the state is not preparing fast enough.
“The worst-case scenario is here, it’s starting already as we’ve seen our number surge into the 700s. There is nothing we have done and nothing that was changed by the governor and by county mayors [Friday] to address what the problems are. Therefore, we are now going to then face the Omicron variant on top of the delta variant with doubling every one and a half to three days, which is going to create a surge that most of us are predicting now that we’re well into the 1,500 to 2,000 a day range by virtue of end of January — if not sooner.”
Hawaii Covid Policy Changes – On Again, Off Again, On Again
Last month, Big Island’s Mayor Mitch Roth took over as the primary emergency rule maker for Hawaii County, as Gov. Ige’s announced Nov.23rd statewide policy change transferred greater Covid policy flexibility for individual County governments.
Mayor Roth’s rules committee are “trying to take a measured approach”, the Mayor’s code for placating all stakeholder interests and priorities, while at the same time and protecting the public health — a public policy balancing act with potential significant consequences for island residents in an on-going and ever changing pandemic threat.
With the governor’s new emergency proclamation went into effect Nov. 24th, and counties are already easing many COVID rules island by island.
- On Oahu, large events and social gatherings will be allowed to operate at 100% capacity. Restaurants, bars and gyms will also no longer have to implement six-foot social distancing requirements.
- Maui County said it is also allowing restaurants and bars to return to full capacity without physical distancing, and lifting all outdoor restrictions. The county added indoor commercial events planned for more than 75 guests will still require an exemption and are encouraged to submit plans early.
- On Hawaii Island, gatherings will now be capped at 25 indoors and 100 outdoors.
- Kauai is also increasing its gathering limits to 40 people indoors and 100 outdoors.
These rule changes come as the governor said he will no longer require county mayors to obtain state approval before enacting emergency rules. County mayors will now be responsible for their own regulations respective to their counties.
Hawaii corrected its Covid-19 vaccination figures on Monday after completing a long-awaited update to its immunization registry that lowered the percentage of the population that has received at least one dose to 77%, and the percentage of Hawaii residents who are fully vaccinated to 71.1%.
Covid / Omicron – News and Latest Developments
The latest variant of SARS-CoV-2 — is steadily working its way through populations with high levels of immunity around the world. There are going to be many coronavirus cases in the coming days and weeks, with little to stop the spread, even if existing immunity can still prevent serious illness.
Initially, being fully vaccinated meant protection against most flavors of infection and their effects.
In the United States, so-called breakthrough cases — infections among the vaccinated — were less common before Omicron, affecting just a small percentage of vaccinated people, by most counts. Now breakthrough cases among the vaccinated are fast becoming the status quo.
The highly contagious Omicron stands to make the notion of a surprise breakthrough infection “completely irrelevant,” said Ali Ellebedy, an associate professor of pathology and immunology at Washington University School of Medicine in St. Louis. This was always bound to happen: As more Americans get vaccinated and more variants circulate, more infections are expected among the vaccinated. But Omicron is speeding up the process.
What we do know about the new Omicron COVID-19 Variant
Omicron’s genetic profile is unique compared with other circulating variants, meaning it represents a new lineage of the virus.
It is distinct from other variants in another crucial way: There are a greater number of mutations. Omicron has more than 30 genetic changes in the spike protein, the part of the virus that binds to human cells, allowing it to gain entry.
Scientists are now sure that those mutations make omicron more transmissible, even among those with a natural or vaccine-acquired immune response. Antibodies defeat the virus by targeting spike proteins, but changes that alter the structure could prevent them from binding as they usually would to neutralize the target. Nonetheless, it is still unknown how the variant acts in real-world situations because it is so new.
In early December, the New York Times first reported the first Omicron cases in the United States have been reported in Colorado, New York, Minnesota and California. and that the Omicron variant had spread to about one-third of U.S. states, while the Delta version remains the majority of COVID-19 infections as cases rise nationwide.
Omicron COVID-19 Variant Can Have Symptoms Similar to the Common Cold
The Omicron variant of COVID-19 is quickly spreading across the United States—and scientists are slowly learning more about the the strain labeled a variant of concern by the World Health Organization (WHO) in late November.
The Centers for Disease Control and Prevention (CDC) recently released a report detailing what the agency has learned from 43 Omicron cases detected in the U.S. between December 1, when the first American case of COVID-19 from Omicron was identified, and December 8.
The CDC data found that 58% of the cases were in people between the ages of 18 and 39. The earliest someone with the Omicron variant developed symptoms was November 15, suggesting that the variant has been in the country for longer than most people realize. Fourteen of the people with COVID-19 cases due to Omicron had traveled internationally within 14 days before they developed symptoms or tested positive for the virus.
The CDC data found that 58% of the cases were in people between the ages of 18 and 39. The earliest someone with the Omicron variant developed symptoms was November 15, suggesting that the variant has been in the country for longer than most people realize. Fourteen of the people with COVID-19 cases due to Omicron had traveled internationally within 14 days before they developed symptoms or tested positive for the virus.
The data found that one patient was hospitalized for two days. No deaths from the Omicron variant have been reported.
Severe Covid infection doubles chances of dying in following year, study finds
Patients who survive severe Covid are more than twice as likely to die over the following year than those who remain uninfected or experience milder virus symptoms, a study says.
The research, published in Frontiers in Medicine, suggests that serious coronavirus infections may significantly damage long-term health, showing the importance of vaccination.
The increased risk of dying was greater for patients under 65, and only 20% of the severe Covid-19 patients who died did so because of typical Covid complications, such as respiratory failure.
The study found that patients who were very unwell with coronavirus had a significantly greater chance of dying over the next year, a trend that was particularly notable among those aged under 65. As these deaths frequently occurred long after the initial infection had passed, they may never have been linked to Covid-19 by the patients’ families or doctors, the study found.
Most of the deaths that occurred in severe Covid-19 survivors were not linked with common complications from the disease – 80% of such deaths occurred for a wide variety of reasons that are not typically associated with the virus.
First Omicron Death Reported; UK
The first verified death from Omicron was reported last October in the UK. The vaccination status of the patient who died has not been reported.
This new research will range from laboratory studies investigating how the virus interacts with antibodies to observations of patient outcomes to large-scale data on infections and hospitalizations. The data will try to answer three key questions, all of which are important to understanding the risk of Omicron.
Three key questions scientists must answer about Omicron and future variants:
- …is whether the variant is more transmissible than the current, prevalent Delta strain. On transmissibility, the data, while early, looks worrisome; Omicron does spread more easily than Delta.
- …does it cause more severe disease. Because the variant is so new, scientists simply do not have adequate trend data yet to determine if the new variant causes more severe disease.
- …will it render our immune defenses — from vaccines and prior infections — less effective. It is extremely unlikely that Omicron will render the Covid-19 vaccines completely ineffective. Omicron has a large number of mutations, including in the spike protein — the part of the protein that the virus uses to bind to and enter human cells. These areas of the protein are critical for vaccine-induced (and infection-induced) antibodies to protect against the virus. However, even small hits to vaccine efficacy will leave us more vulnerable to infection and illness and can make it harder to contain the virus.
- In a new study announced on Monday, researchers from the University of Oxford tested blood samples of people 28 days after their second dose of either the Oxford-AstraZeneca or Pfizer-BioNTech vaccine.
- When omicron was introduced to those samples, scientists reported “a substantial fall” in the neutralizing antibodies that fight off Covid compared to the immune responses seen against earlier variants.
VACCINE DEVELOPMENTS
New data shows Merck’s experimental covid-19 pill is less effective than early results predicted
Drugmaker Merck and its partner Ridgeback Biotherapeutics released data Friday showing their experimental pill to treat covid-19 is less effective than early clinical trials predicted, a finding that emerged as the Food and Drug Administration raised questions about the drug.
The study by the drugmakers found that, among participants receiving the pill, just one participant died during the trial, compared with nine deaths in the placebo group, the companies said in a news release Friday.
Last month, Merck & Co has applied for U.S. emergency use authorization for its tablet to treat mild-to-moderate patients of COVID-19, putting it on course to become the first oral antiviral medication for the disease. AstraZeneca asked U.S. regulators last week to grant emergency use authorization for its experimental drug as a preventative therapy, and today announced positive results from a late-stage study.
Separately, Food and Drug Administration advisors voted unanimously Friday to recommend that the agency authorize a booster shot of the Pfizer-BioNTech coronavirus vaccine six months after vaccination for people 65 years and older and for anyone at risk for severe illness.
Three doses of Pfizer vaccine likely to protect against Omicron infection, early tests suggest
Three doses of the Pfizer/BioNTech vaccine are likely to protect against infection with the Omicron variant but two doses may not, according to laboratory data that will increase pressure to speed up booster program.
Tests using antibodies in blood samples have given some of the first insights into how far Omicron escapes immunity, showing a stark drop-off in the predicted protection against infection or any type of disease for people who have had two doses. The October 2021 findings suggest that, for Omicron, Pfizer/BioNTech should now be viewed as a “three-dose vaccine”.
The vaccine makers said they would continue “at full speed” with plans to develop an updated Omicron-based vaccine by March 2022 if needed – and their working presumption is that it will be.
Moderna says its booster significantly raises the level of antibodies to thwart Omicron
A booster shot of the Moderna coronavirus vaccine significantly raises the level of antibodies that can thwart the Omicron variant, the company announced on Monday.
The news arrives as Omicron rapidly advances across the world, and most coronavirus vaccines seem unable to stave off infection from the highly contagious variant.
Moderna’s results show that the currently authorized booster dose of 50 micrograms — half the dose given for primary immunization — increased the level of antibodies by roughly 37-fold, the company said. A full dose of 100 micrograms was even more powerful, raising antibody levels about 83-fold compared with pre-boost levels, Moderna said.
Both doses produced side effects comparable to those seen after the two-dose primary series. But the dose of 100 micrograms showed slightly more frequent adverse reactions relative to the authorized 50-microgram dose.
Earlier, Moderna’s CEO predicted that existing Coronavirus vaccines would be much less effective at combating Omicron compared with previous variants of the virus, spooking financial markets in the United States, Europe and Asia as scientists rush to learn about the new variant. “There is no world, I think, where [the effectiveness] is the same level … we had with delta,” Bancel said, referring to the highly contagious variant that was first detected in India in late 2020.
“I just don’t know how much, because we need to wait for the data,” he said. “But all the scientists I’ve talked to … are, like, ‘This is not going to be good.”
The world still doesn’t know for sure if omicron is more transmissible than delta (though there’s some preliminary evidence), let alone if it causes more serious disease, but drugmakers continue to sound the alarm that vaccines will need to be tweaked (which means they would be making, and selling, more boosters). But nations will face an Omicron wave with a new weapon: treatments that could help make infections less deadly.
World Health Organization Update
Omicron (COVID-19) variant carries worrisome mutations that may let it evade antibodies, scientists said. But it will take more research to know how it fares against vaccinated people.
Scientific experts at the World Health Organization warned on Friday that a new coronavirus variant discovered in southern Africa was a “variant of concern,” the most serious category the agency uses for such tracking.
The designation, announced after an emergency meeting of the health body, is reserved for dangerous variants that may spread quickly, cause severe disease or decrease the effectiveness of vaccines or treatments. The last coronavirus variant to receive this label was Delta, which took off this summer and now accounts for virtually all Covid cases in the United States.
The W.H.O. said the new version, named Omicron, carries a number of genetic mutations that may allow it to spread quickly, perhaps even among the vaccinated.
Independent scientists agreed that Omicron warranted urgent attention, but also pointed out that it would take more research to determine the extent of the threat. Although some variants of concern, like Delta, have lived up to initial worries, others have had a limited impact.
Omicron first came to light in Botswana, where researchers at the Botswana Harvard H.I.V. Reference Laboratory in Gaborone sequenced the genes of coronaviruses from positive test samples. They found some samples sharing about 50 mutations not found in such a combination before. So far, six people have tested positive for Omicron in Botswana, according to an international database of variants.
State of the Pandemic – 2021 Achieve
October 2021
- The national outlook has improved considerably in recent weeks. Hospitalizations and new case reports have been falling since mid-September.
- More than 700,000 coronavirus deaths have now been reported nationwide. Daily death reports have started to slowly decline, but it remains common for more than 1,800 fatalities to be reported in a day.
- Alaska has, by far, the most recent cases per capita in the country. The spike there has overwhelmed the state’s medical system and forced doctors to make wrenching decisions about who receives the highest levels of care.
- Conditions have improved rapidly in the South, which experienced the worst of the summer case surge. Daily caseloads in Mississippi and Florida have declined by roughly 50 percent over the last two weeks.
- Daily case reports are flat or falling in 40 states, but hotspots have emerged in the northern third of the country, including Montana and Idaho. Parts of Michigan’s Upper Peninsula are reporting their highest caseloads of the pandemic.
- About two-thirds of eligible Americans are fully vaccinated. The daily pace of vaccination has increased somewhat in recent days as Pfizer booster shots became more widely available.
The immensity of our loss’: 650,000 white flags show American lives lost to Covid
A sea of more than 650,000 white flags is lining the National Mall near the Washington monument in the nation’s capitol to represent the American lives lost so far to Covid-19.
As of September 2021, more than 4,645,000 people have died from the coronavirus worldwide. More than 226 million cases have been reported worldwide.
Data compiled by Johns Hopkins University.
The United States continues to have the highest cumulative number of confirmed cases and deaths globally. In September, the U.S. Covid-19 death toll surpassed 667,000. Though cases dipped after January, a new wave began only a few months later, prompting President Biden to urge governors to reinstate mask mandates and other virus-related restrictions. “This is deadly serious,” Biden said in March.
At a certain point, the United States would reach the gruesome milestone of 1 in 500 people dying of covid-19, but the question was when. The answer: 19 months.
President Biden to Require Vaccines for Most Federal Workers and Contractors, Hawaii follows at the state level
- President Biden will sign orders mandating the vast majority of federal workers and government contractors to get vaccinated against the coronavirus.
- Los Angeles is set to become the first major U.S. school district to require vaccinations for students. Here’s the latest on the pandemic
- U.S. states with low vaccination rates see sharp spikes in children with Covid-19
- Hawaii also launched a SMART Health Card app in September that enables residents to store verification of their vaccination status in their phones, in effect a vaccination passport.
Is Delta variant of the virus more dangerous than the earlier variant of Covid-19 from last year?
The New York times reported today the following — “… evidence so far suggests that Delta is similarly severe to earlier versions of the virus, probably with only modest differences in one direction or the other. Delta is certainly more contagious — and its contagiousness does call for some new precautions, like more frequent mask wearing — its severity does not appear to be fundamentally different.”
New coronavirus variant reportedly detected in South Africa
The European Union (27 member countries) will reinstate restrictions on American travelers next month, a change that would primarily affect unvaccinated people, as soaring rates of new coronavirus infections have made the United States a global pandemic hot spot.
As Covid-19 cases surge again, locally and across the U.S., many frustrated people have been asking how to channel the outrage they feel toward those who have refused vaccines. A Washington Post headline summed things up this way: “Vaccinated people are ready for normalcy — and angry at the unvaccinated getting in their way.”
Hawaii coronavirus cases could top 1,000 by end of October if low vaccination rates persist
Based only a 65% vaccination rate, experts say we can expect to see a big jump in the numbers is alarming.
“Unvaccinated” individuals carry the majority of the hospitalization. The peak of daily cases will come, then the peak for hospitalizations will follow about two weeks later.
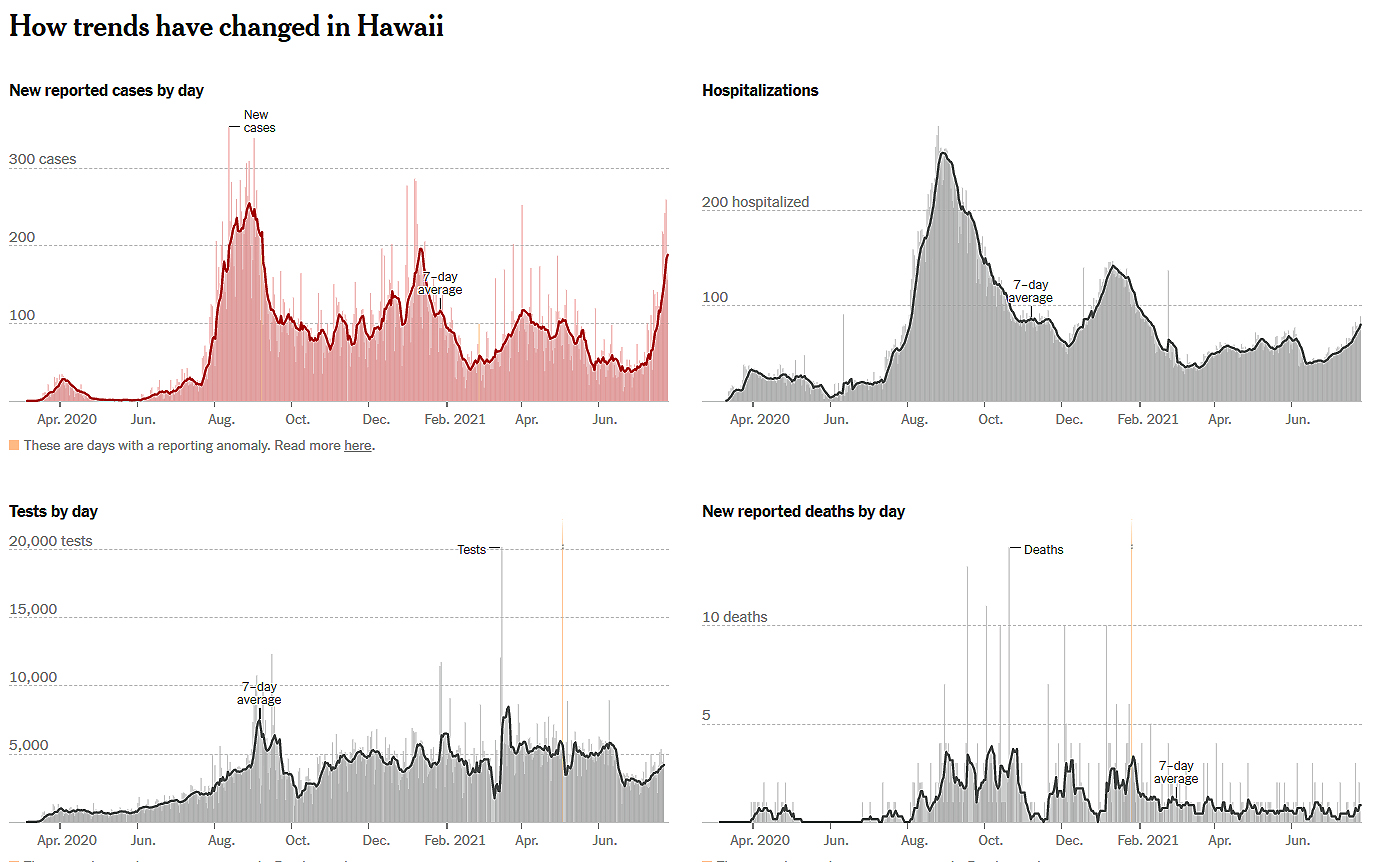
Hawaii Vaccination Update / Global Outlook
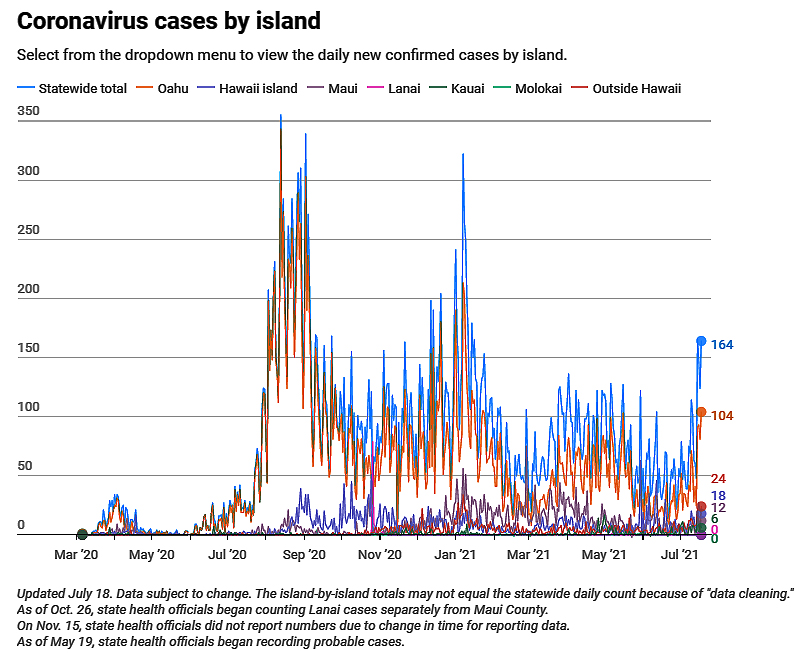
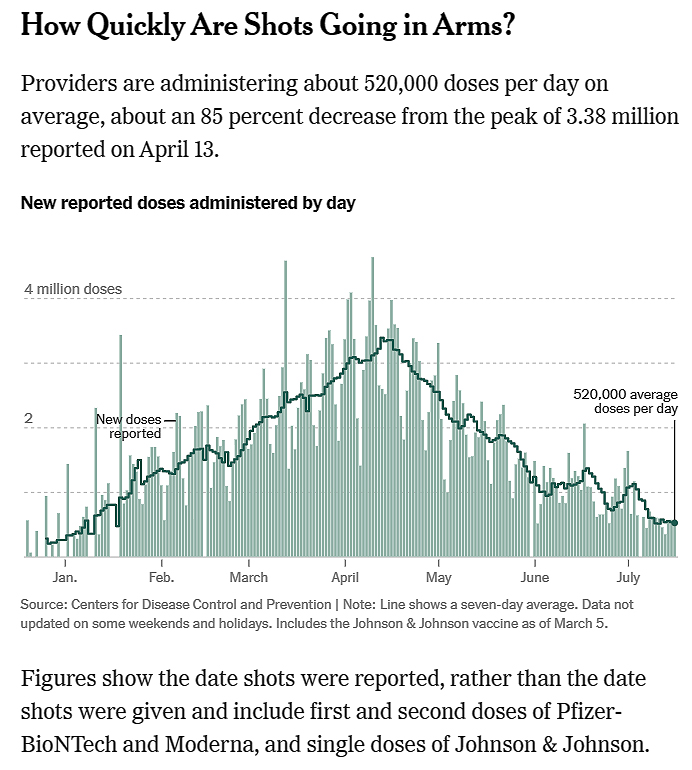
COVID-19 Delta variant spreading rapidly in U.K., now the United States.
News Update —
Just three weeks ago, Great Britain celebrated the success of its vaccination campaign by lifting many coronavirus-related restrictions. “Goodbye, lockdown,” one headline said. But since then, a more transmissible new strain of the coronavirus has taken hold, imperiling plans to fully reopen the country on June 21.
Public health officials in the United States are now grappling with the possibility that a similar regression could take place here and, just as in the U.K., place in jeopardy the end of the pandemic that many had foreseen for this summer.
The potent new variant, known as Delta or B.1.617, emerged in India during that country’s recent coronavirus surge. According to British Health Secretary Matt Hancock, it is around 40 percent more transmissible than the original strain, or wild type, that first appeared in 2019.
While several coronavirus variants have appeared since the start of the pandemic, epidemiologists worry that mutation could create a strain that evades vaccines.
“We cannot let that happen in the United States,” Fauci said, describing the scenario in the U.K. as a “powerful argument” for vaccination. Biden has set the goal of inoculating 70 percent of American adults by the July 4 weekend. Although the nation has now surpassed 300 million doses of coronavirus vaccine administered, the effort has recently slowed.
The emergence of the Delta variant presents a new challenge because, as University of Edinburgh immunologist Eleanor Riley told the Financial Times, vaccines provide “somewhat less protection against infection with the Delta variant.” Even fully vaccinated people appear to develop fewer neutralizing antibodies against the Delta strain than for other variants.
Fauci also said in Tuesday’s briefing that the new variant may be “associated with increased disease severity” compared with the coronavirus wild type.
People who have had only their first dose of the two-dose vaccines from Pfizer and AstraZeneca appear to be especially vulnerable to the Delta variant, Fauci said on Tuesday. (The AstraZeneca vaccine has been widely used in Europe but is not being administered in the United States; the Moderna vaccine, by contrast, is popular in the United States but not in the United Kingdom.) While both vaccines were about 50 percent effective against the original SARS-CoV-2 strain three weeks after the first dose, they were only 33 percent effective against the Delta strain.
Two weeks after the second dose, their effectiveness jumped to 88 percent for Pfizer and 60 percent for AstraZeneca, representing what were only slight decreases in effectiveness when compared with the original coronavirus strain.
Globally, as of 10th of June 2021, World Health Organization reported
380,482 new cases
174,061,995 confirmed cases
3,758,560 deaths
2,154,075,098 vaccine doses administered
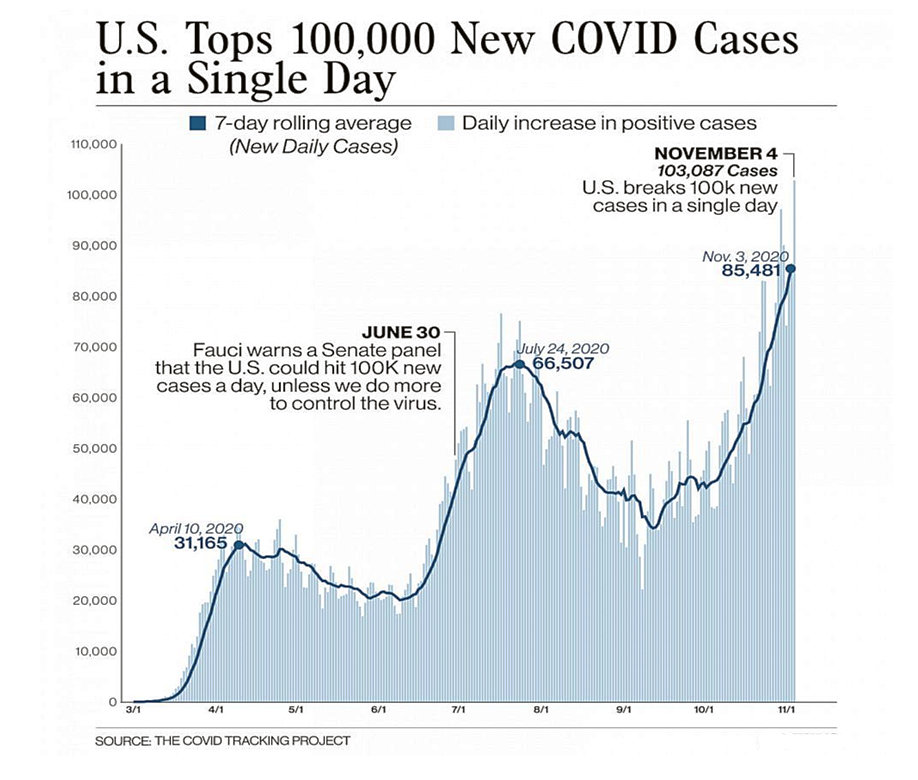 President Trump COVID-19 Legacy
President Trump COVID-19 Legacy
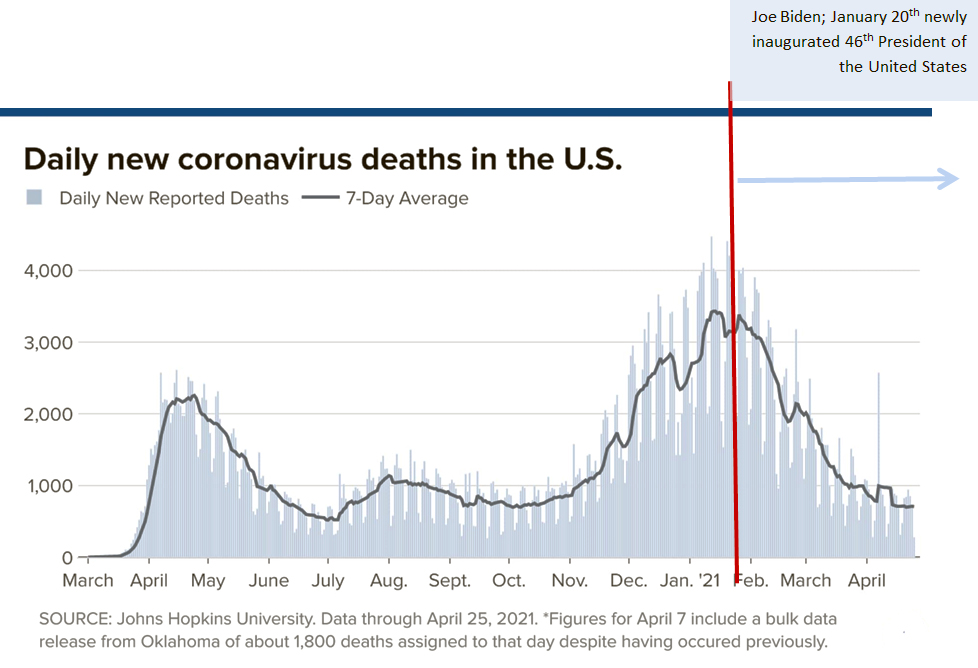
The U.S. reported 4,131 coronavirus-related deaths Wednesday, January 20th 2021, setting a record for the most Covid-19 deaths recorded in a single day (NBC News)
Covid–19 death toll tops 403,596 under President Trump, and as Joe Biden becomes the 46th president of the United States, also on January 20th 2021.
CDC says fully vaccinated Americans can go without masks outdoors
update: April 27, 2021
Federal health officials said Tuesday that fully vaccinated Americans can go without masks outdoors when walking, jogging or biking, or dining with friends at outdoor restaurants.
The guidance from the Centers for Disease Control and Prevention is the latest set of recommendations for people who are two weeks past their final shot and for those who have not yet been inoculated. The guidelines address growing calls from infectious-disease and other public health experts to relax mask mandates for the outdoors because breezes disperse airborne virus particles, distancing is easier, and humidity and sunlight render the coronavirus less viable.
Annual COVID-19 boosters may become the norm
Scientists don’t yet know how long protection from the current cohort of coronavirus vaccines will last. Since the discovery of the original strain in late 2019, the virus has continued to mutate, yielding variants—similar-but-distinctive versions of the virus with the potential to be more infectious, deadly, and escape the antibody safeguards provided by the existing COVID-19 vaccines. To stay ahead of virus evolution, some vaccine creators are racing to design new shots to beat back variants while working to determine how long immunity lasts from current doses.
And the new “normal,” some experts say, could mean routine inoculation, or boosters, against COVID-19.
A booster shot is “a repeat dose of a vaccine that you’ve already received to literally boost your immunity,” says Susan R. Bailey, an allergist and clinical immunologist and president of the American Medical Association. The immune system creates virus-fighting memory from repeat exposure. It’s common that a second or third encounter with an antigen, a molecule that prompts antibody production, creates a “greater and more long lasting” immune response, Bailey says.
The Pfizer-BioNTech and Moderna COVID-19 vaccines, which are mRNA vaccines, include an initial dose and a second shot three or four weeks later, respectively.
Currently, the third COVID-19 vaccine authorized for emergency use in the United States, made by Johnson & Johnson, is given in a single dose, but the company is testing the efficacy of a second booster shot, too. (The U.S. has temporarily paused its distribution of Johnson & Johnson’s current dose, however, as it investigates reports of rare but severe blood clots.)
Third coronavirus vaccine dose likely needed within a year, Pfizer CEO says
Leaving middle seat empty lowers COVID-19 spread on planes
It’s not just about elbow room anymore: Leaving middle seats empty may reduce COVID-19 spread on airplanes, CDC advises. A study, conducted by researchers at the Centers for Disease Control and Prevention (CDC) and Kansas State University, was carried out on flights with blocked-off middle seats. In the United States, only Delta continues to leave middle seats empty, and the airline has announced that the practice will continue only until April 30th.
The CDC recommends against nonessential air travel for those unvaccinated for COVID-19.
Variant and more contagious stains of the COVID-19 virus have firmly established themselves in Hawaii. The Hawaii Tribune-Herald reported that nearly 350 cases of COVID-19 in Hawaii have been caused by a variant strain of the novel coronavirus, fifteen of those variant cases have been identified on the Big Island.
- B.1.1.7, which was originally found in the United Kingdom, has the N501Y mutation that is associated with increased transmissibility. Health data indicates that in places where this virus mutation is discovered it become dominant strain, primarily because it spreads easily and rapidly.
- B.1.351, or the South African variant, has also been identified in some Hawaii cases and is associated with increased transmission, and with the end result that vaccinated persons with protective antibodies, may find their vaccination less effective. Expects agree, the vaccine antibodies are not going to work quite as well against with the the South African variant.
- A recently newly identified virus mutation, the so-called B.1.429, California variant, has also been associated with increased transmission, and vaccine protective antibodies also are “slightly less effective” against this strain.
The current 3 US Vaccines now available work well and provides various degrees of protection, and in all cases , so far, have provided essential protection against all currently identified mutations, avoiding serious health complications and hospitalization, and in the extreme, death.
Statewide, there have been 302 cases of the B.1.429 strain, 37 of the B.1.1.7 and seven cases of the B.1.351, for a total of 346 variant cases, according to data from the DOH.
In Hawaii County, 10 cases of the California variant and five of the U.K. variant have been identified.
CDC issues long-awaited guidance for cruise lines
CDC is preparing the way for the return of Cruise Lines to visiting again Hawaii.
Previously, the Centers for Disease Control and Prevention (CDC) issued an order on January 29, 2021 requiring the wearing of masks by travelers to prevent spread of the virus that causes COVID-19. Conveyance operators must also require all persons onboard to wear masks when boarding, disembarking, and for the duration of travel. Operators of transportation hubs must require all persons to wear a mask when entering or on the premises of a transportation hub.
Are we entering a ‘fourth wave’ of the pandemic? Experts disagree.
POINT — “In terms of the United States, we’re just at the beginning of this surge,” said Osterholm, who is also the director of the Center for Infectious Disease Research and Policy at the University of Minnesota. “We haven’t even really begun to see it yet.”
COUNTER POINTS — Former Food and Drug Administration commissioner Scott Gottlieb predicted the current spikes would not amount to “a true fourth wave,” citing the number of Americans who have already been infected, plus the number of people who have been vaccinated.
“I think that there’s enough immunity in the population that you’re not going to see a true fourth wave of infection,” Gottlieb said. “What we’re seeing is pockets of infection around the country, particularly in younger people who haven’t been vaccinated and also in school-age children.”
Last week, Anthony S. Fauci, the government’s top infectious-disease expert, also cast doubt on the prospect of another national surge, saying vaccines are the X-factor that was absent during the first, summer and winter waves.
Experts do agree that the trends are troubling and that they can be traced to a convergence of factors: increased spread of the more transmissible variants and a broad loosening of public health measures, such as mask mandates and limits on indoor dining.
Biden Pushes Mask Mandate as C.D.C. Director Warns of ‘Impending Doom’
The administration is stepping up the pace of vaccinations and expanding access to shots, but it remains in a race against a virus on the upswing.
President Biden, facing a rise in coronavirus cases around the country, Monday, called on governors and mayors to reinstate mask mandates as the director of the Centers for Disease Control and Prevention warned of “impending doom” from a potential fourth surge of the pandemic.
The president’s comments came only hours after the C.D.C. director, Dr. Rochelle Walensky, appeared to fight back tears as she pleaded with Americans to “hold on a little while longer” and continue following public health advice, like wearing masks and social distancing, to curb the virus’s spread.
The back-to-back appeals reflected a growing sense of urgency among top White House officials and government scientists that the chance to conquer the pandemic, now in its second year, may slip through their grasp. Coronavirus infections and hospitalizations are on the upswing, including a troubling rise in the Northeast, even as the pace of vaccinations is accelerating.
“Please, this is not politics — reinstate the mandate,” Mr. Biden said, adding, “The failure to take this virus seriously is precisely what got us into this mess in the first place.”
New Covid vaccines needed globally within a year, say scientists
Survey of experts in relevant fields concludes that new variants could arise in countries with low vaccine coverage
The planet could have a year or less before first-generation Covid-19 vaccines are ineffective and modified formulations are needed, according to a survey of epidemiologists, virologists and infectious disease specialists.
Scientists have long stressed that a global vaccination effort is needed to satisfactorily neutralize the threat of Covid-19. This is due to the threat of variations of the virus – some more transmissible, deadly and less susceptible to vaccines – that are emerging and percolating.
The grim forecast of a year or less comes from two-thirds of respondents, according to the People’s Vaccine Alliance, a coalition of organizations including Amnesty International, Oxfam, and UNAIDS, who carried out the survey of 77 scientists from 28 countries. Nearly one-third of the respondents indicated that the time-frame was likely nine months or less.
Persistent low vaccine coverage in many countries would make it more likely for vaccine-resistant mutations to appear, said 88% of the respondents, who work across illustrious institutions such as Johns Hopkins, Yale, Imperial College, London School of Hygiene & Tropical Medicine and the University of Edinburgh.
“New mutations arise every day. Sometimes they find a niche that makes them more fit than their predecessors. These lucky variants could transmit more efficiently and potentially evade immune responses to previous strains,” said Gregg Gonsalves, associate professor of epidemiology at Yale University, in a statement.
“Unless we vaccinate the world, we leave the playing field open to more and more mutations, which could churn out variants that could evade our current vaccines and require booster shots to deal with them.”
Pfizer, Moderna vaccines are 90% effective after two doses in study of real-life conditions, CDC confirms
The Pfizer-BioNTech and Moderna vaccines being deployed to fight the coronavirus pandemic are robustly effective in preventing infections in real-life conditions, according to a federal study released Monday.
Centers for Disease Control and Prevention found that the vaccines reduced the risk of infection by 80 percent after one shot. Protection increased to 90 percent following the second dose. The findings are consistent with clinical trial results and studies showing strong effectiveness.
The CDC report is significant, experts said, because it analyzed how well the vaccines worked among a diverse group of front-line working-age adults whose jobs make them more likely to be exposed to the virus and to spread it.
“These findings should offer hope to the millions of Americans receiving coronavirus vaccines each day and to those who will have the opportunity to roll up their sleeves and get vaccinated in the weeks ahead. The authorized vaccines are the key tool that will help bring an end to this devastating pandemic” said CDC Director Rochelle Walensky, who added, “the study shows national vaccination efforts are working.”
Hawaii Virus Update:
228,000 of Hawaii’s residents Complete Vaccination
C.D.C. Says 3 Feet in Elementary Schools With Masks Is OK
In a major policy revision intended to encourage more schools to welcome children back to in-person instruction, federal health officials on Friday relaxed the six-foot distancing rule for elementary school students, saying they need only remain three feet apart in classrooms as long as everyone is wearing a mask.
The three-foot rule also now applies to students in middle schools and high schools, as long as community transmission is not high, officials said. When transmission is high, however, these students must be at least six feet apart, unless they are taught in cohorts, or small groups that are kept separate from others.
The six-foot rule still applies in the community at large, officials emphasized, and for teachers and other adults who work in schools, who must maintain that distance from other adults and from students. Most schools are already operating at least partially in person, and evidence suggests they are doing so relatively safely. Research shows in-school spread can be mitigated with simple safety measures such as masking, distancing, hand-washing and open windows.
“Transmission dynamics are different in older students — that is, they are more likely to be exposed to SARS-CoV-2 and spread it than younger children,” the Centers for Disease Control and Prevention said in a statement.
Teachers’ unions across the country have argued forcefully for six-feet of distancing, and have lobbied the C.D.C. and the Biden administration to maintain the previous guidance.
On Friday, Randi Weingarten, president of the American Federation of Teachers, the nation’s second-largest educators’ union, released a statement saying she would “reserve judgment” on the new distancing guidelines pending further review of research on how the virus behaves in school settings.
Hawaii, one of the leading states in COVID-19 vaccinations.
Hawaii as of Thursday had the eighth-highest rate of administered doses per 100,000 people, according to the U.S. Centers of Disease Control and Prevention. About 40,450 people per 100,000 have received at least one vaccine dose. That’s a total of 572,716 people, according to the CDC.
With more doses coming in, the DOH has opened vaccination efforts to people in Phase 1C, which includes those 65 years and older, essential workers and people with three chronic medical conditions that include dialysis, severe respiratory disease and people undergoing chemotherapy or other infusion therapies.
While focusing on vaccinating people 65 years and older and people with certain medical conditions, the DOH also is making sure to concentrate efforts on people working at hotels, restaurants and bars, which have been drastically affected by the spread of COVID-19. An estimated more 500,000 plus people are expected to be vaccinated inside the category 1C grouping, representing the state’s largest single category. According to DOH, the state presently does not have enough doses to fully open up the 1c qualifying group of the population to vaccinations, instead focusing on essential workers employed at hotels, restaurants and bars, and elder population 65 and up.”
Downtrend in new U.S. infections stalls, fueling concerns over virus variants’ spread
Dr. Anthony Fauci warned against the relaxation of COVID-19 protocols earlier this week. While the baseline of cases has fallen in the US, he said the too soon relaxation could lead to a “rebound.”
- About 70,000 new COVID-19 cases are still diagnosed each day in the US.
Among the nations with overweight populations above the 50 percent threshold were also those with some of the largest proportions of coronavirus deaths — including countries such as Britain, Italy and the United States. Some 2.5 million people have died around the world of covid-19, more than 517,000 of which were in the United States.
CO2 from fossil fuels could exceed pre-pandemic levels
The planet has just a few months to stop carbon emissions surpassing the levels seen before the pandemic, as economies begin to recover and return to burning fossil fuels, according to a global energy watchdog. Data from the International Energy Agency (IEA) found the emissions from fossil fuels began rising steadily in the second half of last year, and levels recorded in December 2020 were 2% higher than in December 2019.
The coronavirus crisis caused the deepest drop in carbon emissions since the end of the second world war, and there were hopes that carbon dioxide output might have peaked in 2019. But the IEA executive director, Dr Fatih Birol, said rising fossil fuel usage was putting these environmental gains at risk, and that if governments did not green up their act, “we may well be returning to our carbon-intensive business as usual”.
U.S. Surpasses 500,000 Covid-19 Deaths, a Monumental Loss of Life
The United States reached a staggering milestone on Monday, surpassing 500,000 known coronavirus-related deaths in a pandemic that has lasted almost a year. The nation’s total virus toll is higher than in any other country in the world. It has far surpassed early predictions of loss by some federal experts. And it means that more Americans have died from Covid-19 than did on the battlefields of World War I, World War II and the Vietnam War combined.
The United States accounts for about 20 percent of the world’s known Covid deaths, but makes up just 4.25 percent of the global population.
About one in 670 Americans has died of Covid-19, which has become a leading cause of death in this country, along with heart disease and cancer, and has driven down life expectancy more sharply than in decades. The losses, monumental for the country, have been searingly personal for the relatives and friends of the 500,000.
U.S. deaths from Covid-19 came faster as the pandemic wore on. The country’s first known Covid-19 death occurred in Santa Clara County, Calif., on Feb. 6, 2020, and by the end of May, 100,000 people had died. It took four months for the nation to log another 100,000 deaths; the next, about three months; the next, just five weeks.
The virus has reached every corner of America, devastating dense cities and rural counties alike through surges that barreled through one region and then another.
500,000 deaths is …
Three times the number of people who died in the U.S. in any kind of accident, including highway accidents, in 2019 (167,127).
More than eight times the number of deaths from influenza and pneumonia (59,120).
More than ten times the number of suicides (48,344).
More than the number of deaths from strokes, diabetes, kidney disease, Alzheimer’s and related causes, combined (406,161).
Only heart disease (655,381) and cancer (599,274) caused more deaths.
When full data for 2020 is available from the Centers for Disease Control and Prevention, Covid-19 will certainly be one of the leading killers.
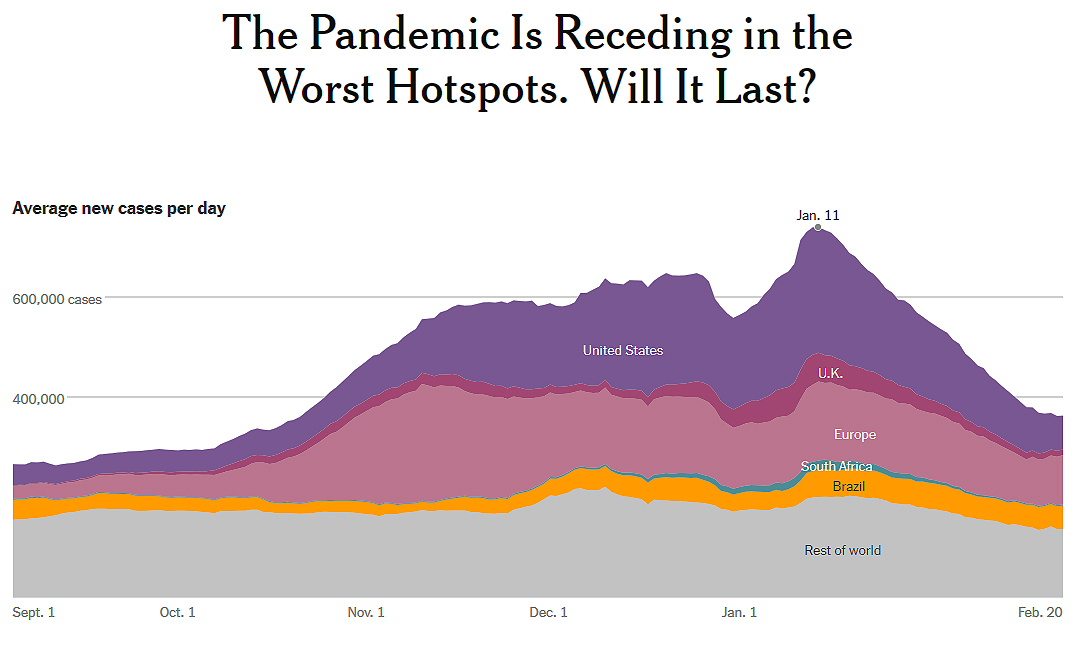
A month ago, the pandemic looked bleak. More than 750,000 coronavirus cases were tallied worldwide in a single day. Infections surged across the entire United States. New variants identified in the United Kingdom, Brazil and South Africa threatened the rest of the world.
Cases are an imperfect measure, and uneven records and testing mask the scope of outbreaks, especially in parts of Africa, Latin America and South Asia. But fewer patients are showing up at hospitals in many countries with the highest rates of infection, giving experts confidence that the decline is real. The lull in many of the world’s worst outbreaks creates a critical opportunity to keep the virus in retreat as vaccinations begin to take effect.
A COVID end in sight for Hawaii?
Lt. Gov. Josh Green (doctor) who serves as Hawaii’s coronavirus preparedness coordinator, says the acute COVID-19 public health crisis could be over in less than three months, and that life may likely start getting back to normal for many residents by summer.
Still, there seems general agreement that many social and recreational activities can probably resume in the spring, although with precautions. “I think you can say the end is in sight,” he said.
Green points to several metrics showing the public health crisis appears to be abating. It’s not just the daily case count, Green said, which had dropped to a seven-day average of 41 as of Friday, according to the Department of Public Health.
Another key number is the infection rate, which is now at 0.8%, and dropping. That means of every 8,000 people tested, fewer than 70 turn out to have the virus, he said. And he predicted the rate soon will be closer to 0.6%.
But now we have vaccines, and that’s a big difference, Green says.
The virus simply won’t have as much chance to jump from person to person and run amok. He projects 350,000 people in Hawaii will have at least started getting vaccines by March 1; 600,000 by April 1; 850,000 by May 1 and more than 1 million by June 1. And as more people get vaccinated, the virus will have fewer available hosts to infect.
Hawaii state’s changing public health policy:
COVID-19 vaccinations, who’s next…
Older Hawaii residents with pre-existing medical conditions that make them vulnerable to severe cases of COVID-19 will likely have to wait another month before vaccines begin rolling out for them, and the same goes for residents in their mid-to-late 60s.
The DOH newest change is allowing people 70 to 75 years old to become eligible sometime in mid-March during the so-called 1b phase. This expanded eligibility, comes with what some call a newly defined group or subset of the previously declared older individuals previously defined as Phase 1c qualified.
Hawaii Department of Health Director Libby Char told lawmakers today, in somewhat vague fashion, that the 1c phase would start in the spring, but precisely when was unclear. Char went onto in her public remarks, that before 1c vaccinations begin, an older subset of eligible 1c group residents will go first, regardless of their health status. At the same time younger people, also scheduled for 1c and with chronic diseases, will just have to wait.
Char stressed Hawaii is “vaccinating the right people as quick as we can,” but she said there have been challenges, including shipping delays caused by winter storms on the U.S. continent.
A new shipment of some 70,000 vaccine doses is expected to help Hawaii make up lost ground this week, she said.
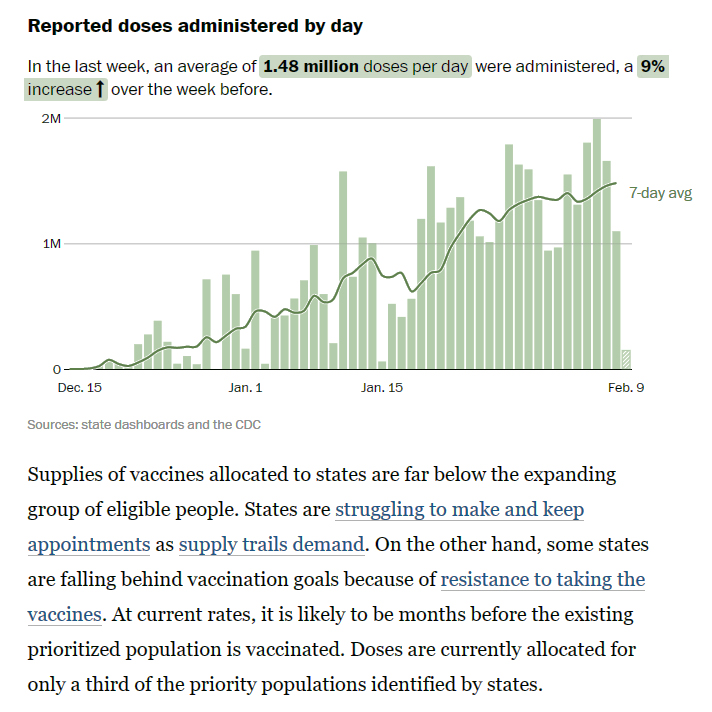
Three million shots a day
Unlike his processor, President Biden has been quite cautious in setting its public vaccination goals. The U.S. presently is averaging 1.7 million COVID-19 vaccinations per day.
Experts now project three million shots per day — probably by April. At that pace, half of adults would receive their first shot by April and all adults who wanted a shot could receive one by June, saving thousands of lives and allowing normal life to return by midsummer.
President Biden told CNN today that anybody who wanted a vaccine would be able to get one “by the end of July.”
Pandemic in retreat?
The number of new coronavirus cases continues to plummet, as does the number of Americans hospitalized with symptoms. 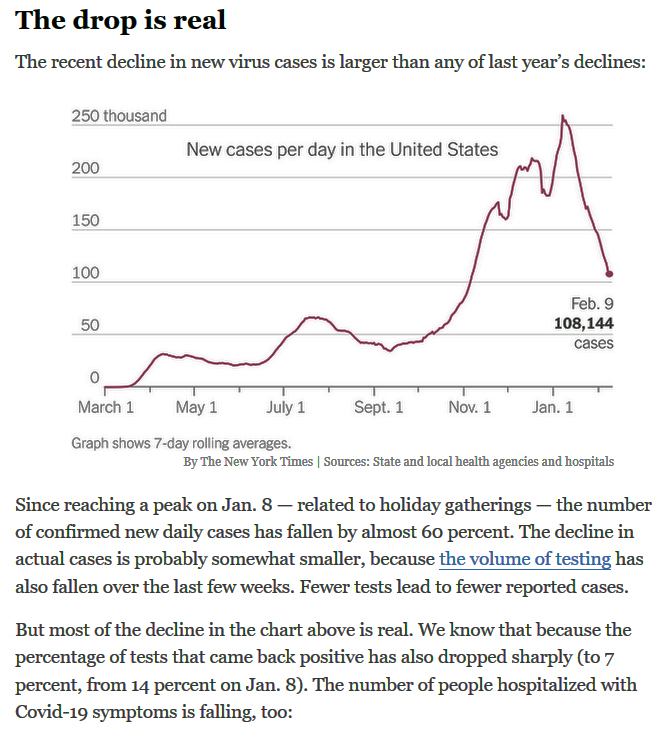
Deaths have also begun to decline. And the number of daily vaccination shots has nearly tripled over the last month.
It’s been a long time since the virus news was as encouraging as it is right now.
The overall situation is still bad. The virus is spreading more rapidly in the U.S. than in almost any other large country, and more than 2,500 Americans are dying daily.
Newly contagious variants may create future outbreaks. For now, though, things are getting better — and a combination of vaccinations, mask wearing and social distancing has the potential to sustain the recent progress.
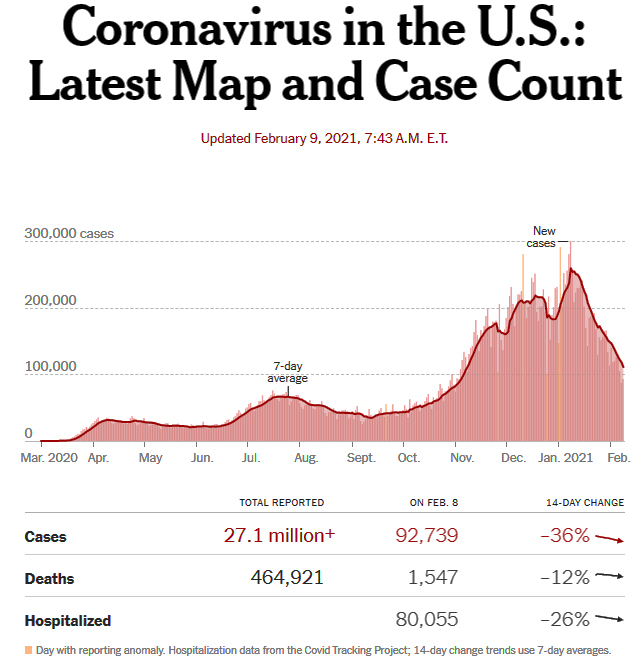
At least 3,255 new coronavirus deaths and 94,893 new cases were reported in the United States on Feb. 10.
Over the past week, there has been an average of 104,559 cases per day, a decrease of 36 percent from the average two weeks earlier.
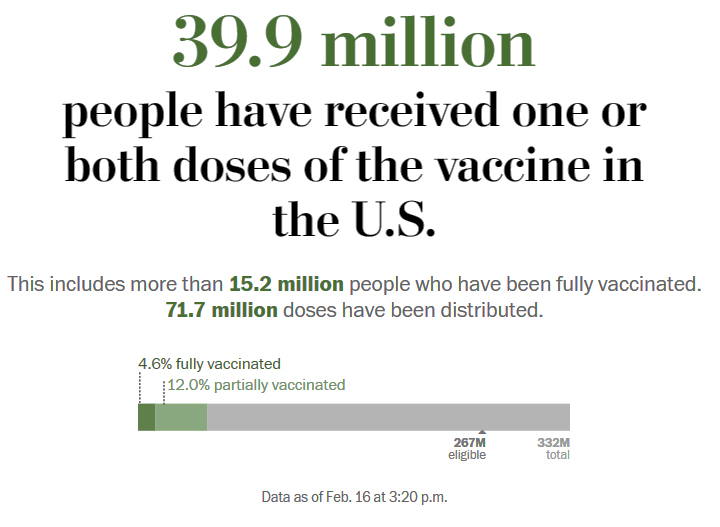
As of Thursday morning, more than 27,328,400 people in the United States have been infected with the coronavirus according to a New York Times database.
- For the first time since Election Day, fewer than 100,000 new cases were announced nationwide daily on Sunday, Monday and Tuesday. Case numbers have been falling rapidly for a month.
- Deaths are also beginning to decrease, though they remain extremely high. Eight states are averaging more than 100 deaths a day.
- The continued spread of variants could threaten the country’s progress in the weeks ahead.
- The pace of vaccination continues to slowly increase, with roughly 1.5 million doses being administered each day.
- States are leaving fewer vaccine doses unused. Through Tuesday, every state but Rhode Island had reported using at least 60 percent of the doses they received.
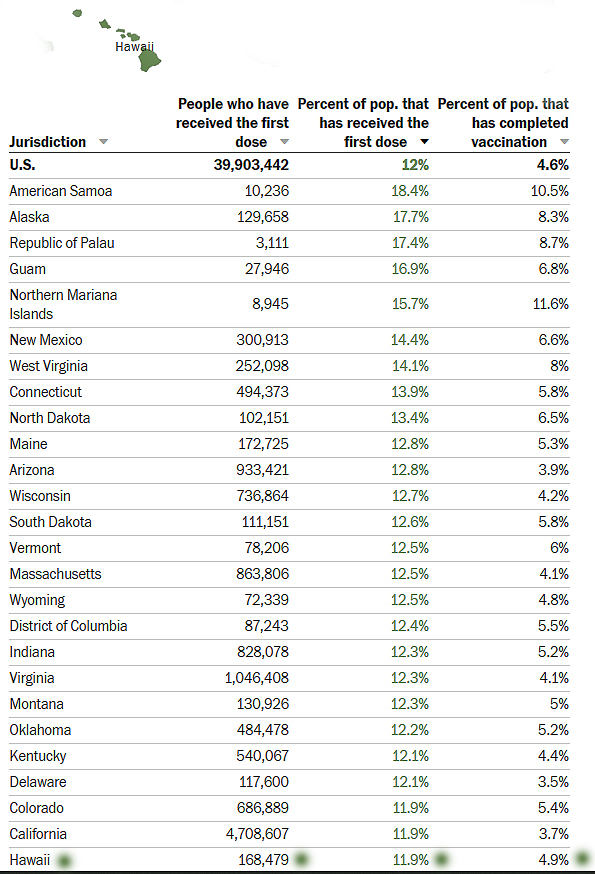
Hawaii trails behind Pacific island territories in the state’s ratio of vaccinations to population. Hawaii ranks 18th in states’ population vaccinated.
Hawaii seniors 75 and older who received their first COVID vaccine during the past 3 weeks are soon scheduled to receive their second (booster) shot — and that has put a squeeze on supplies, limiting others access to the vaccine. Since the kupuna population 75 and older started getting their first doses of the Pfizer vaccine their second doses will be available starting this week. Moderna recipients are expected to receive their second dose staring next week. Hawaii’s Kupuna population 65 – 74 years of age, many with pre-existing conditions placing them at very high risk, will likely have to wait to May- June under Hawaii’s 1c protocol before they qualify vaccination. Many mainland states have set their 1b (Hawaii’s present stage of the vaccination protocol) for 65 years old and older, including California, Oregon, and Washington.
Hawaii Pacific Health and Queen’s Medical Center are prioritizing second dose recipients ahead of first time applicants, in a statewide vaccine environment already taxed by limited vaccine supplies. Tens of thousands of seniors are in the group due for their second doses, limiting the number of people able to get their first dose for the next few weeks.
“It concerns us that we’re going to be limited to mostly doing second shots and not being able to schedule new appointments for first shots,” said HPH CEO Raymond Vara.
Lt. Gov. Josh Green remains hopeful that the federal government will start sending more vaccines to the islands in the weeks ahead. His expectation is that wider distribution of the vaccine will become available by March.
California Runs Out of Vaccine Doses
Braking News – Thursday, 2-11-21
Facing a shortage of coronavirus vaccine doses, Los Angeles will temporarily close five of its inoculation sites, including one of the country’s largest, at Dodger Stadium, raising new questions about the federal government’s handling of supplies and distribution.
By Thursday, the city will have exhausted its supply of the Moderna vaccine for first-dose appointments, Mayor Eric Garcetti said at a news conference. The centers will be closed on Friday and Saturday with plans to reopen by Tuesday or Wednesday of next week, he said.
“We’re vaccinating people faster than new vials are arriving here in Los Angeles,” Mr. Garcetti said. “I’m concerned as your mayor that our vaccine supply is uneven, it’s unpredictable and too often inequitable.”
Early COVID-19 News
Oxford vaccine shown to have only limited effect against South African variant of coronavirus
- Leading vaccine scientists are calling for a rethink of the goals of vaccination programs, saying that herd immunity through vaccination is unlikely to be possible because of the emergence of variants like that in South Africa.
- The comments came as the University of Oxford and AstraZeneca acknowledged that their vaccine will not protect people against mild to moderate Covid illness caused by the South African variant. The Oxford vaccine is the mainstay of the UK’s immunization program and vitally important around the world because of its low cost and ease of use.
U.S. military to help states with coronavirus vaccine sites
- More than 1,000 active-duty military personnel are poised to support state vaccination sites, the White House said on Friday as the Biden administration continues to look for ways to ramp up the national inoculation effort.
- New infections in the United States have dropped 17 percent over the past week, but the daily death toll remains high; in total, more than 454,000 people have died of covid complications nationwide.
- Public health officials have warned Americans to avoid large gatherings on Super Bowl Sunday.
Hawaii’s Department of Health reported Friday the presence of the B.1.1.7 (UK) mutant variant of COVID-19, has been detected in Oahu.
Oxford/AstraZeneca vaccine protects against virus variant dominant in the U.K., but far less effective on South African strain of the virus.
The vaccine developed by Oxford University and AstraZeneca protects against the highly transmissible coronavirus variant that is dominant in the United Kingdom, according to results from ongoing clinical trials in Britain.
Oxford researchers reported Friday that their vaccine was 75 percent effective against the new variant first detected in the U.K., known as B.1.1.7 — compared with 84 percent efficacy against the original strain that appeared here at the beginning of the pandemic.
J&J Vaccine Falls Short in Covid-19 Effectiveness
Johnson & Johnson (NYSE:JNJ) said on Friday that its one-shot coronavirus vaccine failed to demonstrate the extremely high effectiveness that many had hoped to see. The efficacy of J&J’s vaccine came in at 66% in preventing moderate and severe disease, 85% against severe disease alone, and fully effective to prevent hospitalization and death from the virus. Figures differed a bit by geography, including 72% effectiveness in the U.S. and 57% in South Africa, which has seen a recent new variant of the disease come up.
Those numbers are far below Moderna’s 94% and Pfizer’s 96% effectiveness rates. J&J argued that earlier trials didn’t take newly mutated variants of COVID-19 into account, thereby adding an extra challenge for the Johnson & Johnson trials.
Nevertheless, the failure of J&J to come up with a highly effective vaccine that requires just one dose and avoids special handling raises introduces additional unknowns into the nation’s supply and demand response to the coronavirus pandemic.
U.S. vaccine program struggles
During the White House’s coronavirus briefing Friday, Anthony S. Fauci, the U.S.’s top infectious-disease expert said that the United States must do more to halt the spread of coronavirus and framed the spread of variant strains.
— most recently, a variant first identified in South Africa was reported in South Carolina — as a “wake-up call” to ramp up inoculation efforts.
The U.S. continues to struggle with its vaccine rollout; just 6.6 percent of the population has received the first dose of the vaccine since it became available in December.
The Biden administration has set a goal of vaccinating at least 1 million Americans per day, officials reiterated, a pace that the United States has narrowly exceeded over the past week.
The emergence of new, mutant versions of the virus was expected, said Fauci and Rochelle Walensky, the director of the Centers for Disease Control and Prevention, and they warned that more are likely to come. Those mutations also will challenge the ability of existing treatments and vaccines to curb the virus’ spread.
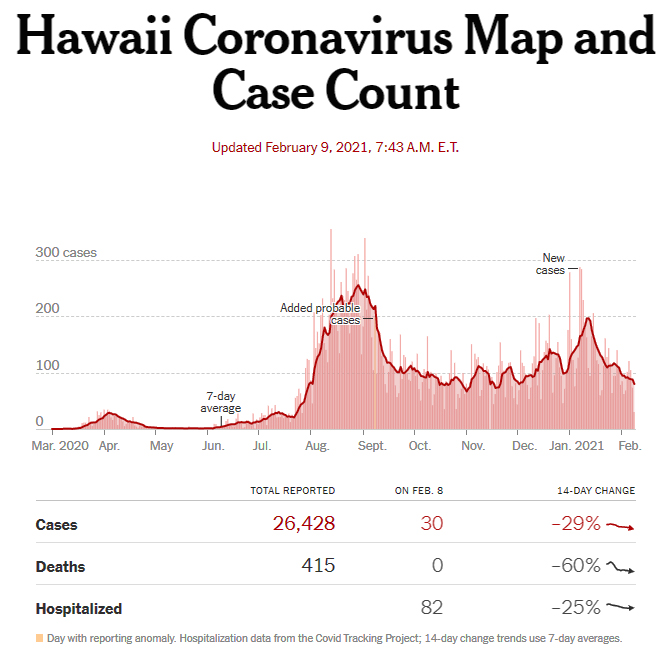
Hawaii Covid-19 Infection and Death Rates Decline in early February
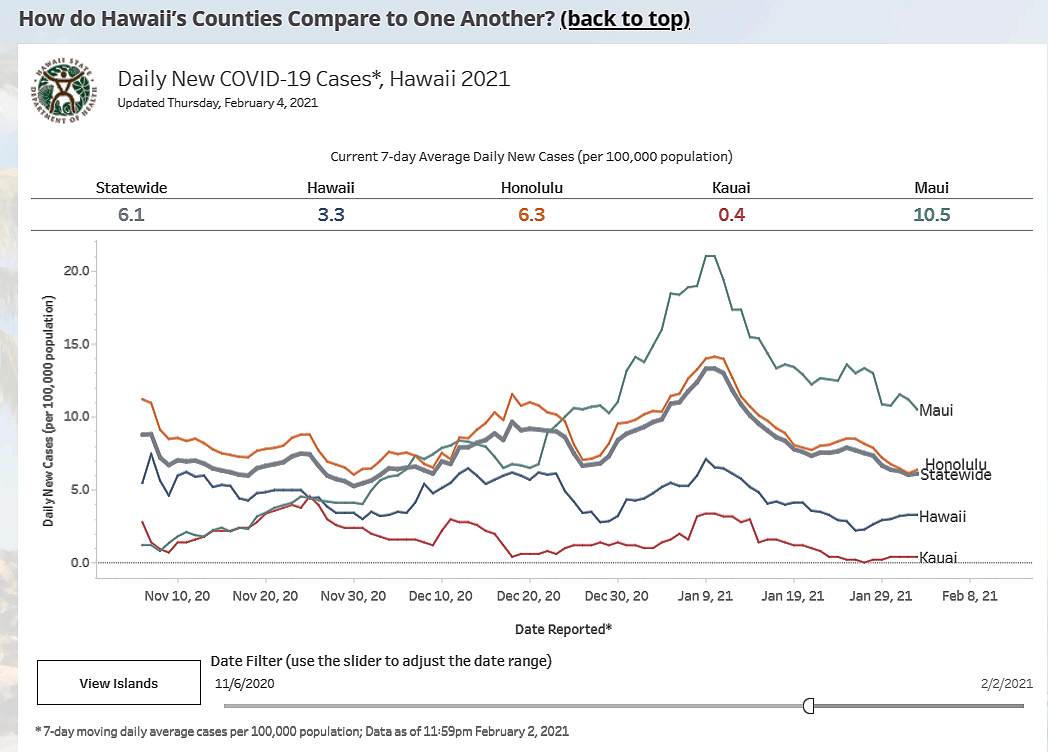
COVID-19 Mutant Variant Linked To California, Finds It Way to Hawaii
DOH reported today that A COVID-19 variant associated with several outbreaks in California has infected one person on Oahu who had traveled to the mainland and a second person on Maui who had not travel to California recently. Hawaii scientists were able to recognize three mutations to the virus’ spike protein — which it uses to enter human cells — characteristic of the variant detected in California.
The mutant virus discovered in Hawaii is known as L452R and is suspected to be associated with increased transmissibility, although further research is needed to verify that assumption.
“What is known is that the prevalence of viral strains with this mutation have greatly increased in California around the same time that case rates in that state have also greatly increased”, Hawaii State Laboratories Division Administrator Edward Desmond said. Hawaii DOH reported 1,656 new infections during the past two weeks.
The state also recorded several COVID-19 infections among people after they got their first of two vaccine doses. Those who have received both doses of the vaccine should expect full immunity approximately two weeks after their second dose.
The vaccines currently being distributed are believed to still be effective in preventing illness, even against the newer strains.
…as of Feb 4, 2021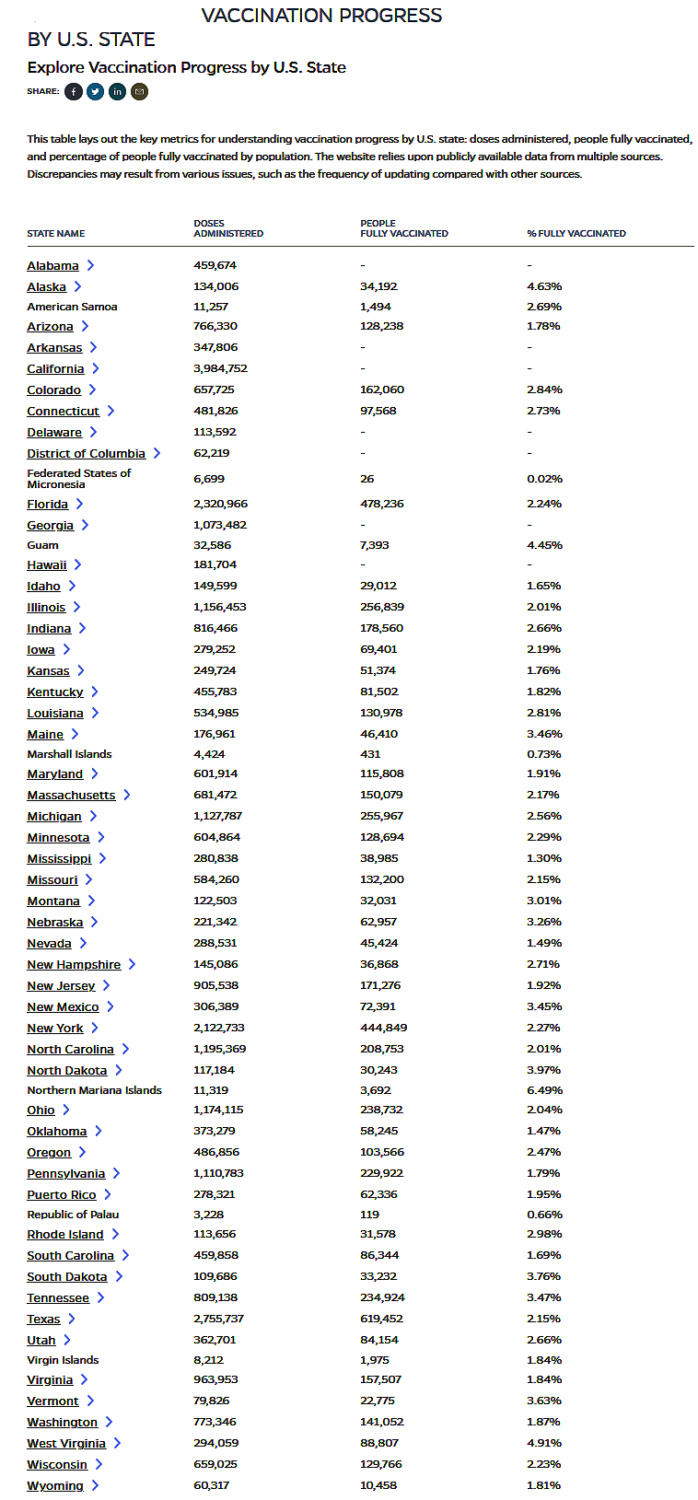
U.S. COVID-19 Death Toll Projected to Reach One-half Million by April; Global Case Count Nears 100 Million, Over 2 Million Dead
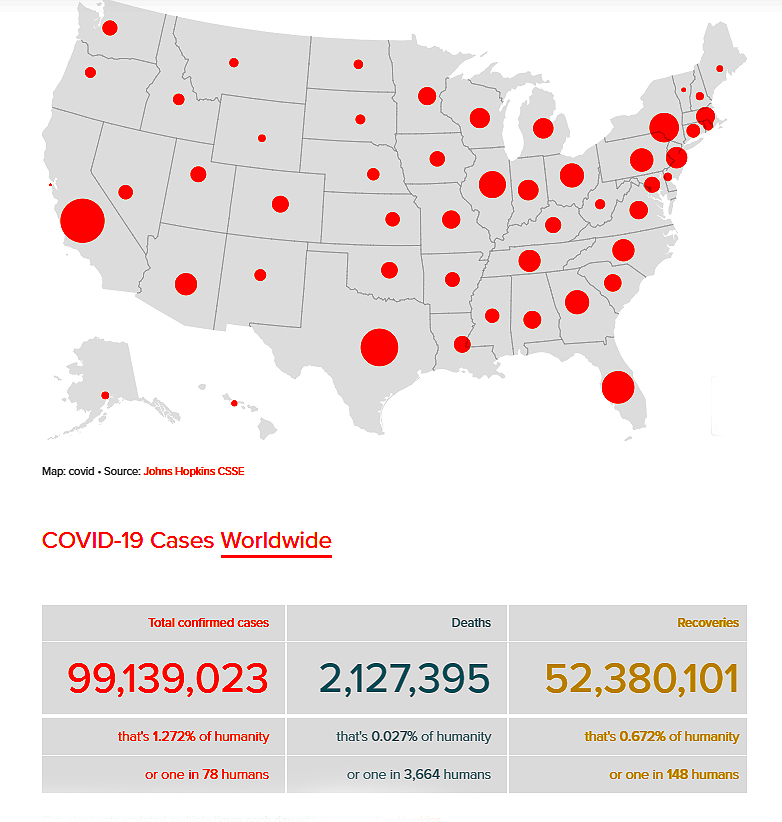
First U.S. case of Mutant COVID-19 virus identified
Just as vaccines begin to offer hope for a path out of the pandemic, officials in Britain on Saturday sounded an urgent alarm about what they called a highly contagious new variant of the coronavirus circulating in England.
On Tuesday of this week, a Colorado man became the first known U.S. case of the newly identified strain of Covid-19 circulating in the UK. The new variant is thought to be far more contagious than the previous strain of COVID-19 in which scientists, the world’s medical community, and governments have built their response assumptions and the current vaccines have been based. Newly established variants have prompted some countries to restrict travel to-from the UK.
 The Colorado man who contracted the new variant, called B.1.1.7, is in his 20s, and had no travel history, according to the state’s health department. In a statement, Colorado Governor Jared Polis said that health officials are conducting an investigation into how the man might have contracted the virus, while he recovers in isolation.
The Colorado man who contracted the new variant, called B.1.1.7, is in his 20s, and had no travel history, according to the state’s health department. In a statement, Colorado Governor Jared Polis said that health officials are conducting an investigation into how the man might have contracted the virus, while he recovers in isolation.
Although the new variant had not been found in the US until now, the Centers for Disease Control and Prevention noted that it was likely already circulating through the country.
The new variant has also recently been detected in at least 17 countries, including South Korea, Spain, Australia and Canada. On Christmas Day, the CDC issued new guidelines for travelers from the UK, requiring proof of a negative Covid-19 test.
All viruses evolve, and the coronavirus is no different. “Based on scientific understanding of viruses, it is highly likely there are many variants evolving simultaneously across the globe,” Mr. McDonald, of the C.D.C., said. “However, it could take weeks or months to identify if there is a single variant of the virus that causes Covid-19 fueling the surge in the United States similar to the surge in the United Kingdom.”
In recent days, the world has watched with curiosity and growing alarm as scientists in the U.K. have described a newly identified variant of the coronavirus that appears to be more contagious than, and genetically distinct from, more established variants.
Citing the rapid spread of the virus through London and surrounding areas, Prime Minister Boris Johnson imposed the country’s most stringent lockdown since March. “When the virus changes its method of attack, we must change our method of defense,” he said.
The British announcement also prompted concern that the virus may evolve to become resistant to the vaccines just now rolling out. The worries are focused on a pair of alterations in the viral genetic code that may make it less vulnerable to certain antibodies.
Viruses mutate all the time. Most of the new variants die out. Sometimes they spread without altering the virus’s behavior. Very occasionally, they trigger dramatic changes.
And the question now facing scientists is straightforward: Does the mutated virus represent an increased health risk? Or has its recent rapid spread through southern England occurred because it has arisen in people who are infecting a lot of other people, possibly because they are ignoring Covid-19 restrictions?
The British variant has 23 mutations, including several that affect how the virus locks onto human cells and infects them. These mutations may allow the variant to replicate and transmit more efficiently, said Muge Cevik, an infectious disease expert at the University of St. Andrews in Scotland and a scientific adviser to the British government.
But several experts urged caution, saying it would take years, not months, for the virus to evolve enough to render the current vaccines impotent.
“No one should worry that there is going to be a single catastrophic mutation that suddenly renders all immunity and antibodies useless,” Dr. Bloom said.
Scientists are worried about these variants, but not surprised by them. Researchers have recorded thousands of tiny modifications in the genetic material of the coronavirus as it has hopscotched across the world.
Some variants become more common in a population simply by luck, not because the changes somehow supercharge the virus. But as it becomes more difficult for the pathogen to survive — because of vaccinations and growing immunity in human populations — researchers also expect the virus to gain useful mutations enabling it to spread more easily or to escape detection by the immune system.
“This thing’s transmitting, it’s acquiring, it’s adapting all the time,” said Dr. Ravindra Gupta, a virologist at the University of Cambridge, who last week detailed the deletion’s recurrent emergence and spread. “But people don’t want to hear what we say, which is: This virus is mutating.”
What we Know So far …
Scientists believe that although initial mutated versions of COVID-19 appear to be more contagious, it does not cause a more severe illness than other established variants. Research is still ongoing, however, and it remains uncertain whether the new variant is actually more transmissible due to a genetic advantage, or whether it is simply spreading so widely due to fluke super-spreader events. A report from Public Health England found that the new variant in the UK has not been linked to higher rates of hospitalization or death.
Is it more contagious than other viruses?
It appears so. In preliminary work, researchers in the U.K. have found that the virus is spreading quickly in parts of southern England, displacing a crowded field of other COVID-19 variants that have been circulating for months. Some scientists have raised the possibility that the increase in transmission is at least partly the result of how it infects children. Normally, children are less likely than teenagers or adults to get infected or pass on the virus. But the new variant may make children “as equally susceptible as adults,” said Wendy Barclay, government adviser and virologist at Imperial College London.
Does it cause more severe disease?
There is no strong evidence that it does, at least not yet. But there is reason to take the possibility seriously. In South Africa, another lineage of the coronavirus has gained one particular mutation. The mutant variant is spreading quickly through coastal areas of South Africa. And in preliminary studies, doctors there have found that people infected with this variant carry a heightened viral load — a higher concentration of the virus in their upper respiratory tract. In many viral diseases, this is associated with more severe symptoms.
Will the variant render the new COVID-19 vaccines ineffective?
Many experts doubt that it will have any great impact on vaccines, although it’s not yet possible to rule out any effect.
The issue is whether the new variant will be able to bypass the protection offered by the Covid-19 vaccines now being administered across Britain and United States.
“If the new variant was going to have a big impact on disease severity, we would have seen that by now,” said Ewan Birney, deputy director general of the European Molecular Biology Laboratory and joint director of its European Bioinformatics Institute in Cambridge.
The U.S. Food and Drug Administration has authorized two vaccines, one from Moderna and the other from Pfizer and BioNTech. Both vaccines create immunity to the coronavirus by teaching our immune systems to make antibodies to a protein that sits on the surface of the virus, called spike. The spike protein latches onto cells and opens a passageway inside. Antibodies produced in respone to the vaccines stick to the tip of the spike. The result: The viruses can’t get inside.
It is conceivable that a mutation to a coronavirus could change the shape of its spike proteins, making it harder for the antibodies to gain a tight grip on them. The mutations include eight in the spike gene. But our immune systems can produce a range of antibodies against a single viral protein, making it less likely that viruses can easily escape their attack.





It is likely the spike protein on the surface of the virus is not altered, otherwise, it may not attach well. No attachment no infection. My guess is the antibodies and T cells that learn to recognize the spike protein via the vaccine will remain effective. If not we know how to make mRNA vaccines very quickly. Science will save us from ourselves yet.